Thyroxine EIA – Ideal for Metabolomics
- ≤ 5 μL Serum or Plasma Sample: for duplicate measurements
- No Extractions Needed
- Validated for Multiple Sample Types: Plasma, Serum, Urine, Fecal Extracts, Media and Dialysates
- High Quality and Economical
- All with superior 4°C Liquid Stability
Metabolomics involves the characterization of small molecule metabolites found in an organism, increasingly used in health applications such as pharmacology, pre-clinical drug trials, toxicology, transplant monitoring, newborn screening and clinical chemistry. The fact that the human metabolome is not yet well characterized presents a key limitation in its use, however. In contrast to the fully sequenced and freely accessible human genome available in the field of genomics, metabolomics remains at an earlier stage of discovery. There are approximately 2900 endogenous or common metabolites in the human body that can be detected in various tissue or biofluid based on the specific functions or metabolic roles they serve.
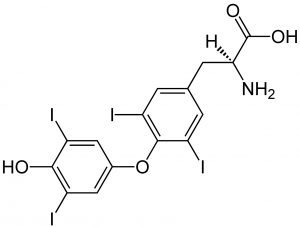
Thyroxine Structure
Thyroxine is the main hormone produced by the thyroid gland. The thyroid hormones, triiodothyronine (T3) and thyroxine (T4), are tyrosine-based hormones primarily responsible for regulation of metabolism. Because iodine is critical to the production of T3 and T4, a deficiency of iodine decreases production of T3 and T4, and may lead to enlargement of the thyroid tissue and development of the disease known as goiter.
The major form of thyroid hormone in the blood is T4, which has a longer half-life than T3. The ratio of T4 to T3 released into the blood is roughly 20 to 1. T4 is converted to the active T3 (three to four times more potent than T4) within cells by deiodinases (5’-iodinase). T3 and T4 are further processed by decarboxylation and deiodination to produce iodothyronamine and thyronamine. Because all three isoforms of the deiodinases are selenium-containing enzymes, dietary selenium is essential for T3 production.
Hypothyroidism is the condition that results from under-production of thyroxine by the thyroid gland, either because the gland is naturally underactive or because radioiodine therapy or surgery for an overactive gland result in underactivity. Thyroxine is taken to replace the deficiency that exists in such situations and to restore T4 metabolic activity. Thyroid hormone production is regulated via the pituitary protein thyrotropin (TSH), which modulates T4 prohormone secretion by the thyroid gland.
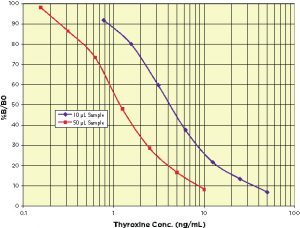
Our Thyroxine Dual Range EIA (K050-H1 and K050-H5) kits allow T4 to be measured using 2μL of sample serum or plasma. Serum or plasma samples are treated with an equal volume of a special Dissociation Reagent that liberates the T4 from any binding proteins. The mixture is then diluted 1:10 or greater with supplied assay buffer and added directly to the well of the provided microtiter plate. The EIA provides results in 90 minutes. The Dual Range formats span either 50 to 0.781 ng/mL with 10 μL of diluted sample, or 4 to 0.0625 ng/mL with 100 μL of diluted sample. This allows T4 levels of 1,000 down to 3.2 ng/mL in serum to be measured on as little as a few μL of sample. Typical human T4 serum levels range from 50 to 125 ng/mL.
Typical Thyroxine EIA Standard Curves
RELATED PRODUCTS
Glucose Colorimetric Detection Kit K039-H
Glucose Fluorescent Detection Kit K039-F
Oxytocin CLIA Kits K048-C
Triiodothyronine (T3) EIA Kit, K056-H
Galactose Colorimetric Detection Kit, K042-H1